Category: Rigid Hammertoes
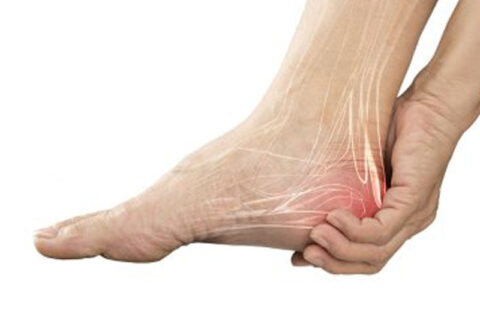
You might be familiar with the carpal tunnel, which is the narrow passageway located at the wrist. The tarsal tunnel is a similar, narrow space,…
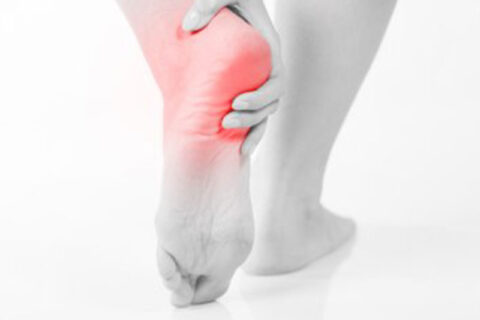
Plantar fasciitis is a common and painful condition that affects the plantar fascia, the ligament that runs from the heel along the bottom of the…
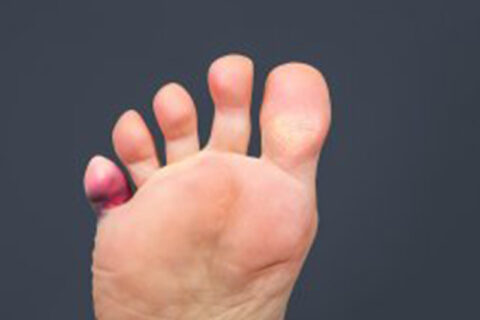
Do you suffer from hammertoes? This condition can cause the muscles and connective tissues in the toes to contract, making the toes bend at a…