Category: Advanced Foot and Ankle Specialists
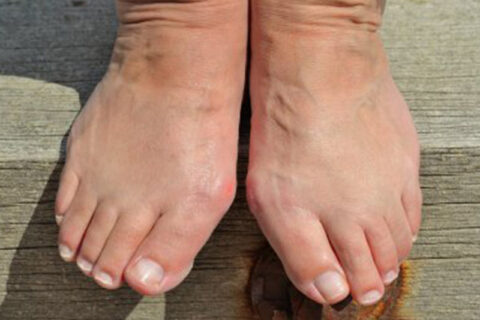
Understanding Morton’s Toe
Your foot has five long bones that connect each toe to the midfoot. These bones are called metatarsals. Your big…
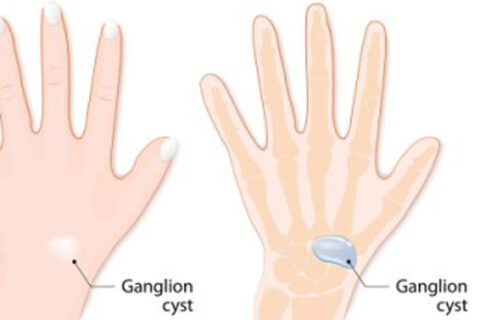
are benign, fluid-filled lumps that appear just below the skin. If you develop one on your foot, your doctor may recommend an aspiration to…
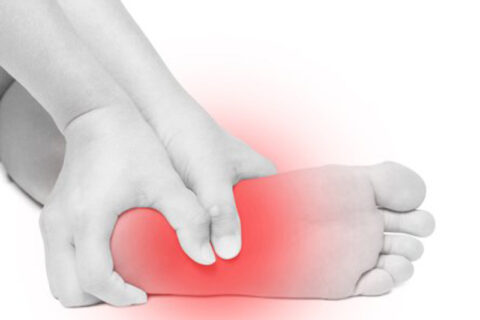
Exercise may be essential for healthy living, but not to the point that you’re exercising while injured. If you experience unusual foot pain,…
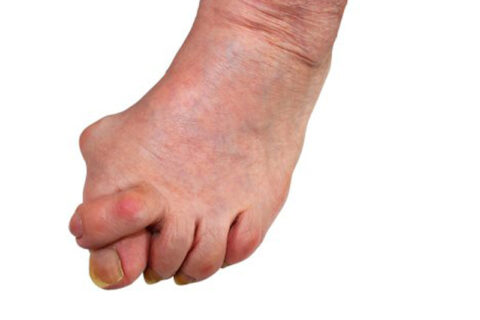
Bunion surgery is the only way to correct this painful foot deformity. Unfortunately, it’s possible for the surgery to fail, and for the…
It’s possible for a podiatrist to detect changes associated with diabetes before you do. Foot doctors serving the Sugar Land area are always on…
Surgery is a common strategy podiatrists use to correct health problems with the feet. Because recovery time from foot surgery can be lengthy,…
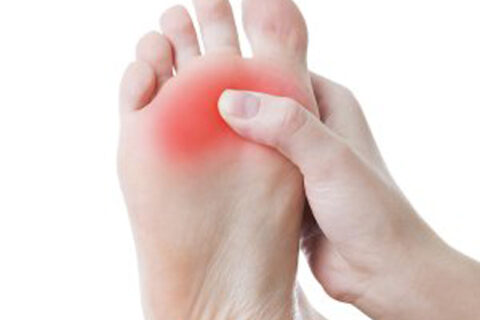
If you’re suffering from foot pain, a neuroma could be to blame. Neuromas, which are also known as pinched nerves or nerve tumors, are benign…
After being diagnosed with diabetes, a podiatrist in Sugar Land will become an important member of your care team. Foot doctors are experts in…
Bunions can be quite frustrating for patients, especially when they’ve already had bunion surgery once. It isn’t uncommon for initial bunion…
Foot pain is common during pregnancy, especially during the third trimester. Since staying physically active is important during pregnancy, consider…